At a glance
Overview
CDC assesses that the season's highest combined peak hospitalizations due to COVID-19, influenza, and RSV to date occurred during the week ending January 3, 2026. However, additional increases in national hospitalization rates for one or more viral respiratory diseases remain possible.
As of March 6, 2026, the amount of acute respiratory illness causing people to seek healthcare is at a low level. The Respiratory Illnesses Data Channel has weekly updates about current trends in respiratory illness. CFA provides weekly epidemic trend estimates for COVID-19, influenza, and RSV.
CDC publishes respiratory disease season outlooks to provide health officials and decision-makers with information to assist in public health preparedness during the fall and winter respiratory virus season (defined as October through mid-May). This includes expectations for when hospitals might experience the most demand due to COVID-19, influenza, and RSV. Our assessments are based on expert elicitation; historical data for COVID-19, influenza, and RSV; and scenario modeling conducted by the Center for Forecasting and Outbreak Analytics (CFA), the COVID-19 Scenario Modeling Hub, and the Flu Scenario Modeling Hub.
We do not anticipate producing additional respiratory disease outlook updates during the remainder of the 2025-2026 season. We continue to monitor respiratory diseases and will provide an update should we identify any unusual events, such as significant resurgence of respiratory disease or the emergence of a new variant of SARS-CoV-2, the virus that causes COVID-19, with moderate to high immune escape properties.
Combined peak hospitalization burden this season
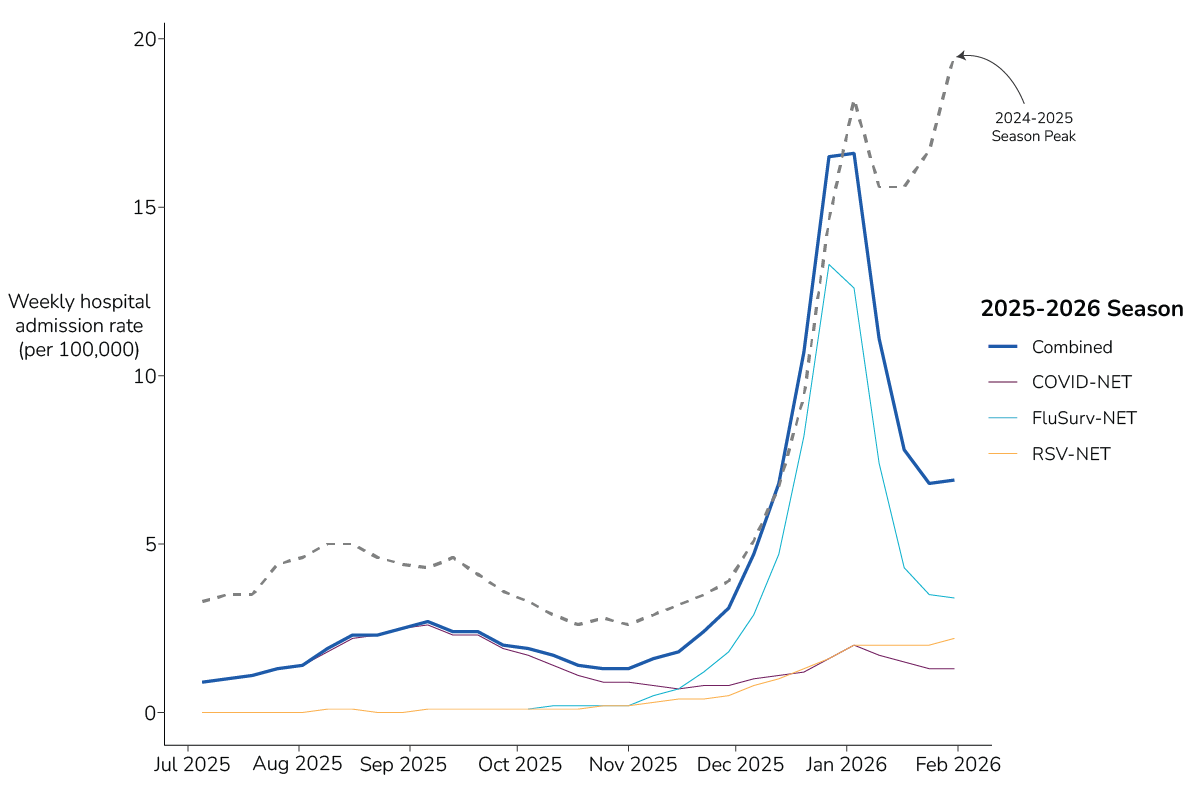
In our initial 2025-2026 outlook, published in August 2025, we anticipated that the fall and winter respiratory disease season would likely have a similar number (within 20%) of combined peak hospitalizations due to COVID-19, influenza, and RSV compared to last season. As of March 6, the season's highest combined hospitalization rate for COVID-19, influenza, and RSV occurred in the week ending January 3, 2026, with 16.6 hospitalizations per 100,000. This was lower than, but within 20% of, the peak weekly hospitalization rate during the 2024-2025 respiratory disease season (19.5 hospitalizations per 100,000 during the week ending February 1, 2025) (Figure 1, RESP-NET).
- COVID-19: As of March 6, the peak hospitalization rate due to COVID-19 occurred during the week ending January 3, 2026, with 2.0 hospitalizations per 100,000. This peak hospitalization rate was substantially lower than the peak that occurred last season (4.2 hospitalizations per 100,000, week ending January 4, 2025), which differed from our outlook in December that the peak would be similar to last season.
- The 2025-2026 fall and winter respiratory disease season marks the first season with minimal COVID-19 activity in some parts of the country since COVID-19 emerged during the 2019-2020 fall and winter respiratory disease season. States that did not experience a substantial winter COVID-19 wave may experience higher levels of summer transmission due to reduced population immunity.
- Influenza: As of March 6, seasonal influenza activity remains elevated nationally. Influenza A activity is decreasing in most areas of the country while trends in influenza B activity vary by region. As of February 28, CDC's in-season severity assessment framework classified this season as moderate across all ages, consistent with the original outlook. Influenza made up the majority of the combined number of COVID-19, influenza, and RSV hospitalizations during the peak week (week ending January 3, 2026) (Figure 1).
- Influenza A (H3N2) viruses are the most frequently reported influenza viruses so far this season. Among 1,507 influenza A(H3N2) viruses collected since September 28, 2025, that underwent additional genetic characterization at CDC, 92% belonged to subclade K.
- RSV: As of March 6, RSV activity is elevated and increasing in some areas of the country. The estimated hospitalization rate due to RSV for the week ending February 21, 2026, is 3.2 hospitalizations per 100,000. This hospitalization rate is similar (within 20%) to the peak that occurred last season (3.9 hospitalizations per 100,000, week ending January 4, 2025). The estimated hospitalization rate for the week ending February 28, 2026, is 3.0 hospitalizations per 100,000. The overall peak hospitalization rate due to RSV may not have occurred yet for the 2025-2026 season.