Purpose
- This document outlines key actions that state, tribal, local, and territorial (STLT) health officials may take to improve jurisdictional readiness to respond to human cases of New World screwworm (NWS) infestation.
- Public health officials should use this document to assess their jurisdiction’s readiness for NWS response, identify potential response gaps, coordinate with jurisdictional response partners, and develop strategies for improving readiness, including requesting technical assistance from CDC if needed.
Background
New World screwworm (NWS) is a species of fly, Cochliomyia hominivorax, that lays its eggs in wounds or other body cavities (e.g., the nose, ears, mouth, eyes, genitals) of warm-blooded animals. The larvae (maggots) feed on living flesh. Although most cases are identified in livestock, NWS can infest any warm-blooded animal, including wildlife, pets, and people. NWS was historically present in the United States but was eradicated in the 1960s following a concerted effort by the U.S. Department of Agriculture (USDA) using the sterile insect technique. The most recent outbreak of NWS in the United States occurred during 2016–2017 in Florida; a collaborative response, involving federal, state, and local government agencies, successfully re-eradicated the flies from the state. Over several decades, the United States also worked with other countries to eliminate NWS from Mexico and Central America. It remains endemic in Cuba, Haiti, the Dominican Republic, and some countries in South America.
NWS has recently resurged across Central America and Mexico, with animal and human infestations reported in every country in the region, threatening incursion into the United States. Rapid identification and prompt public health investigation of NWS infestations in people will support appropriate clinical management and timely implementation of control measures to prevent establishment or further spread of the flies.
Key actions to improve readiness
Apply the One Health approach to operational planning and response through collaboration with your state agriculture and wildlife officials, and other relevant partners.
- Discuss preparedness plans and information sharing for both human and animal cases of NWS with your State Public Health Veterinarian (SPHV), State Animal Health Official (SAHO), and other jurisdictional One Health partners (e.g., state department of agriculture, state fish and wildlife management agency, state department of natural resources).
- Consider instituting a routine communication cadence with One Health partners, as appropriate for your jurisdiction’s NWS and other One Health preparedness and response activities.
- Identify which agency or agencies have jurisdiction over companion animals, should a case of NWS be identified. If no single state agency has jurisdictional authority over companion animals, STLT public health officials should collaborate with jurisdictional agencies to collectively determine responsibilities for activities regarding companion animals.
- Coordinate with jurisdictional One Health partners to ensure aligned response efforts.
- Coordinate with the SPHV, SAHO, state wildlife officials, and other local One Health partners to identify a communication structure for sharing NWS detection data for human and animal cases and related material. Some jurisdictions have had success with establishing mutual data-sharing agreements between One Health partners.
- Remain engaged with federal interagency partners on established communication platforms (e.g., Screwworm.gov, STLT and Federal One Health Update call series) to stay informed of United States government NWS response coordination and activities.
- Examples of information regarding human cases that might inform animal health investigation activities include locations (e.g., ZIP codes) where the patient visited, lived, or stayed during the timeframe when the infestation was active; presence of any animals in these locations; whether the larvae were disposed of properly and how, or in which geographic location, larvae may have escaped a wound; or, if the larvae were thrown in the trash, where that trash was taken (e.g., landfill). This information will help federal and state One Health partners identify priority locations for NWS fly trapping and surveillance activities.
- STLT should coordinate with jurisdictional One Health partners to discuss escalation criteria for an Incident Command System (ICS) structure and agency engagement should an ICS structure be established. Some jurisdictions have had success in strengthening One Health coordination in an ICS structure by: embedding a public health liaison in an animal health–led response structure; embedding an animal health liaison in a public health–led response to a human case; or placing a One Health lead in the respective response structures to enhance interagency and external coordination and collaboration.
- Coordinate jurisdictional NWS planning and preparedness with local and tribal health departments, depending on state public health governance structure.
- Federally recognized tribes and tribal epidemiology centers are public health authorities and should be engaged proactively in the reporting process.
- Engage and help educate human healthcare providers in your jurisdiction to make them aware of NWS, when to suspect it, and what they should do if they suspect a case. STLT health officials can contact newworldscrewworm@cdc.gov for more information on available resources that can be shared with human healthcare providers.
- Understand the process and data flows for 1) reporting and evaluating suspected cases, 2) initiating the NWS Case Report Form for confirmed cases in One CDC Data Platform (1CDP), and 3) investigating confirmed cases and completing the NWS Case Report Form in 1CDP (see Case reporting, investigation, and response below).
- Be familiar with the CDC case investigation guide and case report form. If you need these documents, contact newworldscrewworm@cdc.gov. Also see the NNDSS eShare September 2025 Webinar: NWS Response (9/16/2025).
- State health departments should identify a point of contact for NWS surveillance and reporting, along with other STLT staff who will need access to the NWS module in 1CDP. To obtain access, the state epidemiologist or designee should email newworldscrewworm@cdc.gov using the subject line “NWS 1CDP Access” and include the following information for each user: name, email address, role (e.g., job title or role for NWS in your jurisdiction), and their 1CDP user status (i.e., if they already have access to 1CDP or not).
- Establish a plan for investigating potential human cases of NWS and notify CDC within 24 hours of identifying a case under investigation (email newworldscrewworm@cdc.gov or, if after regular business hours, contact the CDC Emergency Operations Center Watch Desk at 770-488-7100).
Ensure collection of appropriate specimens and establish processes with the State Public Health Laboratory (SPHL) to submit human specimens for species confirmation and notification of results.
- Designate a point of contact for NWS at the SPHL and include this information in outreach to healthcare providers.
- Be familiar with the process for specimen handling and submission as outlined in Clinical Overview of New World Screwworm.
- Consider procuring leakproof containers, 70% ethanol, zip-top plastic bags, and packaging materials available to support specimen shipping and submission, and larvae and egg disposal.
- Understand the data flow for NWS human case reporting internal process for sharing NWS specimen identification results with other relevant STLT staff in your jurisdiction, once results are received from CDC’s Diagnostic Parasitology Laboratory.
- Ensure One Health coordination is established between the SPHL and the State Animal Health Diagnostic Laboratory.
- Be familiar with the process for proper disposal of larvae not sent for specimen identification and reporting procedures for improperly discarded specimens. If STLT partners cannot confirm that all larvae were disposed of properly, share information about where larvae may have escaped or were discarded (e.g., landfill) with USDA. They will need to know the location to set up fly traps for surveillance.
- Consider making a list of public and private waste disposal sites for household or medical non-hazardous waste or establish contact with the appropriate waste management and/or hazardous waste authorities in your jurisdiction.
- Engage and educate human healthcare providers in your jurisdiction about appropriate disposal of larvae not sent for specimen identification.
- Identify populations potentially at higher risk if NWS is found in the U.S. (e.g., people who spend a lot of time or sleep outdoors). The groups at risk may vary based on the most likely NWS scenarios for your jurisdiction (e.g., people who spend a lot of time or sleep outdoors). Consider your jurisdiction's location, climate, population density, and animal characteristics.
- Consider engaging partner groups that may be able to facilitate education on recognizing NWS infestation and implement occupational health and safety measures for populations at higher risk.
Case reporting, investigation, and response
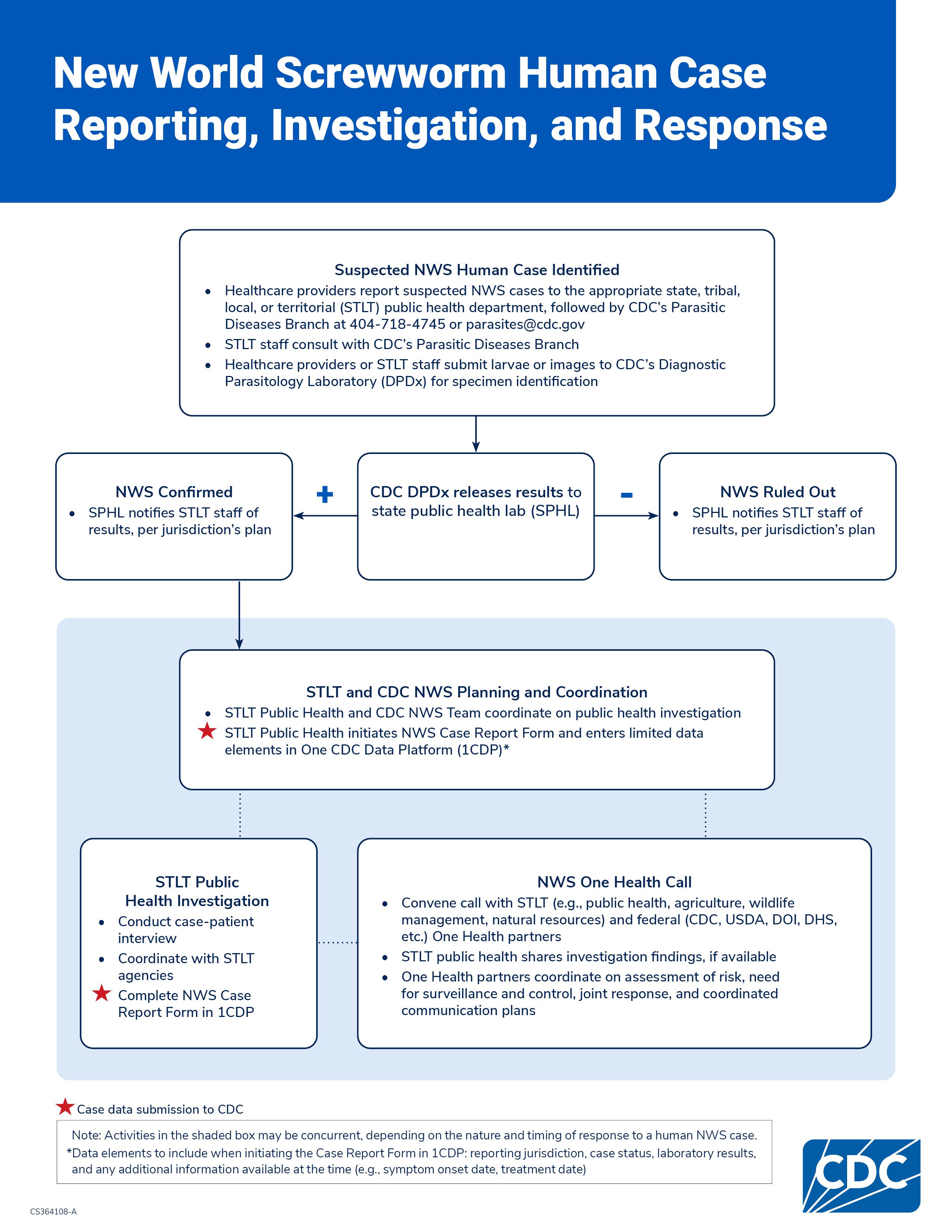
Communication planning
Prepare for public messaging
- Engage jurisdictional (public health, agriculture, wildlife), federal (CDC, USDA, DOI), and other relevant One Health partners in public communication planning and discuss interagency coordination for messaging regarding human cases of NWS, animal cases of NWS, and USDA control activities (e.g., setting traps for fly surveillance or sterile fly releases). This applies to suspect or confirmed cases in humans or animals, as applicable.
- Preplan for communication needs related to:
- Case identification
- Media notices
- Local county/municipality messaging
- Appropriate treatment of NWS infestations in humans
- Differences in messaging around travel-associated versus locally acquired NWS human infestations
- Language translation, if needed
- Ensure public health risk communication messages reach communities of focus and populations at greatest risk in your jurisdiction.
- Consider engaging outreach groups, such as non-governmental organizations working with unhoused people or their companion animals or agricultural workers, home care and food delivery services, or similar organizations.
Points of contact
CDC
Clinical inquiries and patient management
parasites@cdc.gov or 404-718-4745
After-hours inquiries
CDC’s Emergency Operations Center at 770-488-7100
- Laboratory identification inquiries
- Instructions for telediagnosis image submissions
- Instructions for physical specimen submissions
Non-clinical questions
State and large-city public health departments
CSTE: Epi-On-Call Phone Numbers
Veterinarians
Report any suspicious animal cases to your USDA Animal and Plant Health Inspection Service (APHIS) Area Veterinarian in Charge and to your SAHO as applicable under state reporting regulations.
