Key points
- Most cases of cat scratch disease (CSD) can be diagnosed based on clinical presentation with compatible cat exposure.
- Laboratory testing for B. henselae is generally unnecessary for CSD but can be helpful for severe or atypical cases.
- CSD is usually self-limited but antibiotic treatment may reduce symptom duration. Severe cases and immunocompromised patients should be treated with antibiotics.
Overview
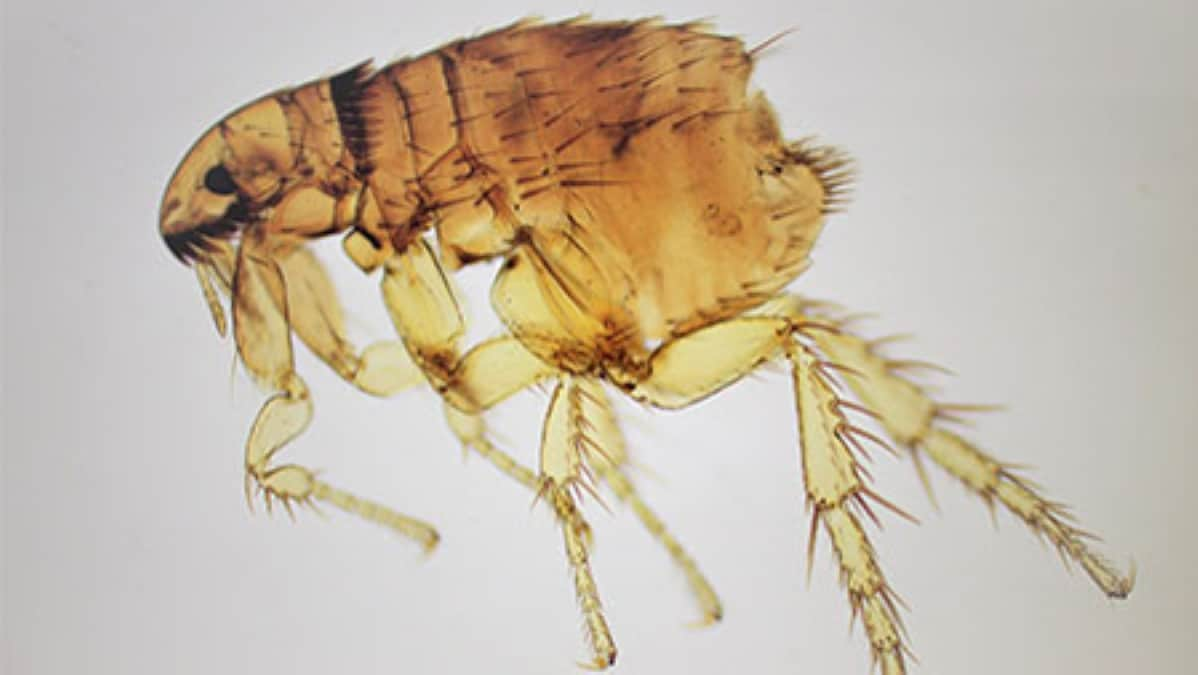
People become infected with B. henselae from the scratch of domestic or feral cats, particularly kittens. Cats can have fleas that carry B. henselae bacteria, which can be transmitted from a cat to a person during a scratch that is contaminated with flea feces. Bartonella henselae infection or CSD disproportionately affects children under the age of 15, though it can affect people of all ages.
Testing and diagnosis
- CSD may be diagnosed clinically in patients with typical signs and symptoms and a compatible exposure history.
- Bartonella henselae is a fastidious, slow-growing bacterium. Cultures should be held for a minimum of 21 days. It is often helpful for healthcare providers to alert the microbiology laboratory that B. henselae is suspected to optimize conditions for growth.
- Serology can aid the diagnosis of CSD, although cross-reactivity with other Bartonella species may limit interpretation. Providers should be aware that serological tests do not reliably differentiate among Bartonella species and positive results may persist for years even after effective treatment.
- Bartonella henselae DNA may be detected by molecular assays of lymph node aspirates or blood, though sensitivity of these methods is not optimal for blood samples. However, lymph node aspiration is not generally recommended except to relieve severe pain and swelling or in cases where the diagnosis is unclear.
- Patients with endocarditis from B. henselae infection often have negative blood cultures (culture-negative endocarditis), which can make diagnosis challenging. When damaged heart valves need to be surgically replaced, excised heart valve tissue can be tested by molecular assay to confirm infection with B. henselae.
Treatment
CSD requires antibiotic treatment if the patient is immunocompromised. Antibiotic treatment of otherwise healthy patients is sometimes recommended depending on patient and provider preference and symptom severity. A short course of azithromycin has been shown in one small study to decrease lymph node volume more rapidly than when there is no treatment. Nevertheless, overall health outcomes in this study were not found to differ between treated and untreated patients.
Disseminated CSD such as retinitis, peliosis hepatis, and endocarditis, require longer treatment courses often with more than one antibiotic. Macrolides, doxycycline, rifampin, and aminoglycosides have all been shown to be effective in treating B. henselae. Consult with an infectious disease expert about treatment options for these presentations.
