Key points
- Many pathogens can cause acute pharyngitis with a rash.
- A scarlet fever diagnosis requires testing for group A Streptococcus.
- Treat scarlet fever with antibiotics to help prevent complications and spread to others.
Overview
Scarlet fever, also called scarlatina, is caused by pyrogenic exotoxin-producing Streptococcus pyogenes (group A strep bacteria).
The incubation period of scarlet fever is approximately 2 to 5 days.
Risk factors
Anyone can get scarlet fever, but age and close contact can increase someone's risk of infection.
Age
Scarlet fever is most common among children 5 through 15 years of age. It's less common in children younger than 3 years of age.
Close contact
Close contact with another person with scarlet fever or other group A strep infection is the most common risk factor for illness.
Crowded settings can increase the risk for spreading the bacteria. These settings include:
- Child care centers and schools
- Detention or correctional facilities
- Homeless shelters
- Military training facilities
Clinical features
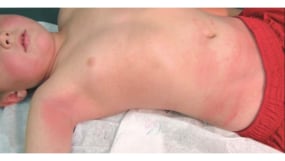
Scarlet fever is characterized by a scarlatiniform rash and occurs with the following group A strep infections:
- Pharyngitis (most common)
- Pyoderma
- Wound infections
Rash characteristics
Characteristics of the rash typically include:
- Erythematous rash that blanches on pressure
- Sandpaper quality
- Pastia's lines, an accentuation of the red rash in flexor creases
- Begins on the trunk and quickly spreads outward
- Usually spares the palms and soles
The rash usually persists for about one week and desquamation may follow.
Other symptoms
The face may appear flushed and the area around the mouth may appear pale (i.e., circumoral pallor). A yellowish white coating with red papillae may initially cover the tongue. The eventual disappearance of the coating can result in a "strawberry tongue."

Diagnosis
Differential diagnosis
The differential diagnosis of scarlet fever with pharyngitis includes multiple viral pathogens that can cause acute pharyngitis with a rash.
Testing and diagnosis
To confirm scarlet fever with pharyngitis, healthcare providers can use
- A rapid antigen detection test (RADT)
- A nucleic acid amplification test (NAAT)
- Throat culture
Healthcare providers can consider a positive RADT, NAAT, or throat culture as confirmation of scarlet fever. Because RADTs are generally less sensitive (more often produce false negatives) than the other tests, a throat culture is recommended after a negative RADT for certain patients.
Testing considerations
Children older than 3 years and adolescents: Compared to people of other ages, children in this age range have higher rates of scarlet fever and increased risk of developing acute rheumatic fever following untreated streptococcal infections.
Thus, for children in this age range, healthcare providers:
- Should test when scarlet fever is suspected
- Consider following up a negative RADT with a throat culture
Have a mechanism in place to contact the family and initiate antibiotics if the back-up throat culture is positive.
Children less than 3 years old: Both scarlet fever and acute rheumatic fever are less common among children in this age group. Testing is most useful when the index of suspicion is high (e.g., a toddler with a fever, sandpaper-like rash, an older sibling with recent streptococcal pharyngitis).
Adults: Throat culture after a negative RADT isn't routinely indicated. Rates of scarlet fever are lower and acute rheumatic fever is very rare among adults.
Treatment
Patients with scarlet fever, regardless of age, who have a positive streptococcal test need antibiotics. Patients without a positive test shouldn't be treated with antibiotics.
Benefits of antibiotics
Using a recommended antibiotic regimen to treat scarlet fever:
- Shortens the duration of symptoms
- Reduces the likelihood of transmission to close contacts
- Helps prevent complications such as otitis media and throat abscesses
Recommended antibiotics
Penicillin or amoxicillin is the antibiotic of choice to treat scarlet fever.
Penicillin V, oral
- Children: 250 mg twice daily or 3 times daily for 10 days
- Adolescents and adults: 250 mg 4 times daily or 500 mg twice daily for 10 days
Amoxicillin, oral
- 50 mg/kg once daily (maximum = 1000 mg) for 10 days
- Alternate: 25 mg/kg (maximum = 500 mg) twice daily for 10 days
Benzathine penicillin G, intramuscular
- Weight less than 27 kg: 1 dose (600,000 U)
- Weight 27 kg or more: 1 dose (1,200,000 U)
Other options for patients with a penicillin allergy
Prescribe one of multiple recommended regimens for patients with a penicillin allergy. However, avoid cephalexin and cefadroxil in patients with immediate-type hypersensitivity to penicillin.
Cephalexin, oral
- 20 mg/kg/dose twice daily (maximum = 500 mg/dose) for 10 days
Cefadroxil, oral
- 30 mg/kg once daily (maximum = 1 g) for 10 days
Clindamycin, oral
- 7 mg/kg/dose 3 times daily (maximum = 300 mg/dose) for 10 days
Azithromycin, oral
- 12 mg/kg once daily (maximum = 500 mg) for 5 days
Clarithromycin, oral
- 7.5 mg/kg/dose twice daily (maximum = 250 mg/dose) for 10 days
Antibiotic resistance
There's never been a report of a clinical isolate of group A strep bacteria that's resistant to penicillin. However, resistance to azithromycin, clarithromycin, and clindamycin can occur and varies geographically and temporally.
Complications
Rarely, complications can occur after scarlet fever.
Suppurative complications
Suppurative complications result from local or hematogenous spread of the organism. They can include:
- Cervical lymphadenitis
- Peritonsillar abscesses
- Retropharyngeal abscess
- Otitis media
- Invasive group A strep disease
Nonsuppurative sequelae
When occurring with group A strep pharyngitis, nonsuppurative sequelae of scarlet fever include:
Post-streptococcal glomerulonephritis can also occur after scarlet fever associated with group A strep skin infections.
These complications occur after the original infection resolves and involve sites distant from the initial group A strep infection site. They're thought to be the result of the immune response and not of direct group A strep infection.
Prevention
Hand hygiene
Good hand hygiene and respiratory etiquette can reduce the spread of group A strep bacteria.
Antibiotic treatment
After at least 12 hours of treatment with an appropriate antibiotic, someone's ability to transmit group A strep bacteria is reduced.
People with scarlet fever should stay home from work, school, or daycare until both of the following are met:
- They are afebrile
- It's been at least 12–24 hours after starting appropriate antibiotic therapyA
Resources
General resources
Amoxicillin shortage: Antibiotic options for common pediatric conditions
Information about PANDAS Physicians Network
Information on antibiotics for treatment of sore throat in children and adults
Diagnosis guidelines
Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis
Infectious Diseases Society of America
2025 Clinical practice guideline update on group A streptococcal pharyngitis: Risk assessment using clinical scoring systems in children and adults
Infectious Diseases Society of America
Red Book: Group A streptococcal infections
American Academy of Pediatrics
Prevention guidelines
Prevention of rheumatic fever and diagnosis and treatment of acute streptococcal pharyngitis
American Heart Association
- Per the American Academy of Pediatrics Red Book 2024–2027, children with group A strep infections should not return to school or a childcare setting until well appearing and at least 12 hours after beginning appropriate antibiotic therapy. In certain scenarios, such as an infection in a healthcare worker or in a group A strep outbreak setting, staying home for at least 24 hours after beginning appropriate antibiotics should be considered.
