At a glance
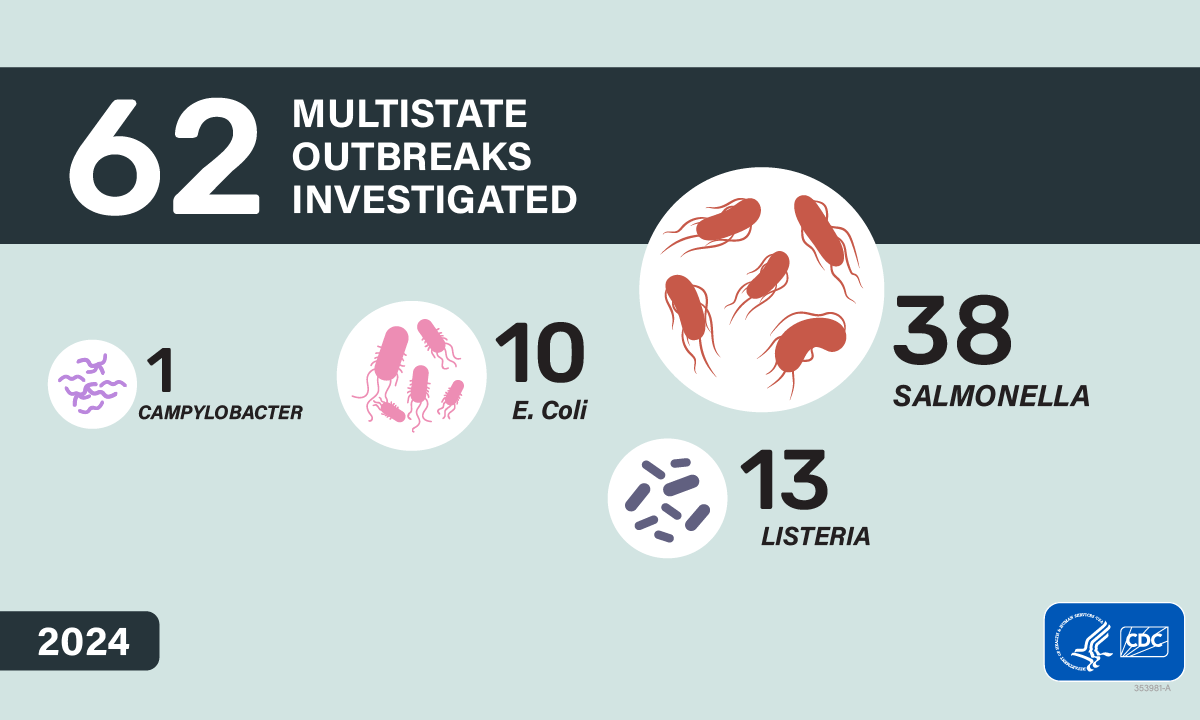
- In 2024, 62 enteric outbreaks were confirmed by CDC and state and regulatory public health partners.
- Outbreak investigators solved 45 of these outbreaks by identifying suspected or confirmed sources.
- Of the solved outbreaks, 29 were foodborne and 16 were linked to animal contact.
- Most of these outbreaks were caused by vegetable row crops, chicken, dairy, and backyard poultry.

Key findings
During 2024, CDC, with state and regulatory public health partners, investigated 203 possible multistate outbreaks, of which 62 were determined to be outbreaks.
- Outbreak investigators solved 45 of the 62 outbreaks (73%).
- Investigators identified a suspected source for 17 outbreaks and a confirmed source for 28 outbreaks.
- The 62 multistate outbreaks caused 2,605 illnesses, 861 hospitalizations, and 36 deaths.
- Contaminated food caused 29 of the 45 solved outbreaks and 1,533 illnesses, 519 hospitalizations, and 19 deaths.
- Animal contact caused the remaining 16 solved outbreaks and 663 illnesses, 191 hospitalizations, and 2 deaths.
- Vegetable row crops, chicken, and dairy caused the most solved foodborne outbreaks (4 outbreaks each). Seeded vegetables caused by far the most illnesses during 2024 (754).
- Backyard poultry caused both the most solved outbreaks (11) and the most outbreak-associated illnesses (532) of any animal contact category in 2024, a 53% reduction in illnesses compared to 2023.
Outbreak investigations at a glance
Highlighted outbreaks

Why this outbreak was notable
The U.S. Food and Drug Administration (FDA) banned the sale of small turtles (those with shells less than 4 inches in length) in the 1970s because of the risk Salmonella infections, especially in children. Although cases significantly declined after the ban, outbreaks continue.
In 2024, there were three different outbreaks of Salmonella Stanley, Salmonella Poona, and Salmonella Sandiego linked to small turtles. Almost one-third of ill people in these outbreaks were young children under the age of 5. Sick people reported purchasing turtles from a variety of locations, including online, at souvenir shops, from street vendors, and at flea markets. All three outbreaks were genetically related to turtle-associated outbreaks investigated in previous years, demonstrating the ongoing nature of turtle-associated salmonellosis outbreaks as the illegal sale of small turtles as pets continues.
What happened as a result
CDC posted an outbreak notice about two of these investigations to inform the public about the risk associated with small turtles, give tips for picking the right pets, and provide information on how to be safe around turtles.
As a result of these investigations, CDC categorized the Salmonella Stanley outbreak strain as a Reoccurring, Emerging, or Persisting (REP) strain, as it has persistently caused illnesses since 2021. The outbreak strain of Salmonella Poona was already classified as a REP strain. This classification allows CDC and partners to track strains over time and collaborate on continued prevention activities outside of acute outbreaks.

Why this outbreak was notable
In July 2024, a state public health department identified a patient infected with an uncommon Salmonella serotype who reported owning pet snakes. Testing revealed genetically related Salmonella in the patient's snakes. By the end of 2024, investigators identified 28 additional cases across 21 states, most involving people who had contact with pet snakes. However, the diversity of snake species, sources of purchase, and long duration of ownership among patients suggested that the snakes themselves were unlikely to be the source for this outbreak. Instead, traceback investigations of feeder rodents used to feed the snakes revealed that patients had purchased rodents from retailers supplied by two common distributors. Feeder rodent testing did not result in the outbreak strain, but this did not rule out feeder rodents an outbreak source given that testing was limited in scope.
This outbreak underscores the human health risks associated with contact with feeder rodents. Patients may have acquired Salmonella through direct handling of feeder rodents, contact with their snakes following ingestion of infected rodents, or indirect exposure via cross-contaminated surfaces or objects in the household environment.
What happened as a result
As a result of this investigation, one major rodent supplier upgraded its biosecurity protocols, including irradiation and a "test and hold" policy to ensure products tested negative for Salmonella before shipment. No cases reported purchases linked to this supplier after those changes.
CDC encouraged pet industry representatives to update their best practices for the feeder rodent industry to recommend irradiation as a standard prevention measure.

Why this outbreak was notable
In 2024, the largest Listeria outbreak linked to deli meat in over 20 years resulted in 65 illnesses, 64 hospitalizations, and 10 deaths. In addition, a Listeria outbreak was linked to pre-cooked meat and poultry products that resulted in 24 illnesses, 22 hospitalizations, and the death of 3 newborns. Both outbreaks were linked to types of ready-to-eat meat and poultry products.
What happened as a result
CDC has existing prevention strategies for people at greater risk for Listeria infection and
- Is conducting focus groups to refine consumer messaging of the prevention strategies.
- Launched a consumer survey to better understand whether consumers identify themselves as at risk for listeriosis and if they are aware of current messaging for people at higher risk to avoid or heat deli meats to 165°F.
Results from these studies will help improve consumer messaging.

Why this outbreak was notable
In 2024, there were 4 outbreaks linked to cheese:
- 3 Listeria outbreaks linked to soft cheeses made with pasteurized milk, including 2 queso fresco-type cheeses and 1 Ecuadorian cheese,
- An STEC O157 outbreak linked to a raw milk cheddar cheese.
Raw milk and pasteurized milk cheeses have been linked to outbreaks in the past. In particular, soft cheeses have been repeatedly linked to Listeria outbreaks.
What happened as a result
CDC conducted focus groups on Listeria and soft cheeses and used findings to update advice for people at increased risk for Listeria infections, including prevention strategies and safer food options.
These strategies include avoiding unheated queso fresco-type cheeses and any type of cheese made with raw milk and instead choosing safer options like other types of cheese, or heating queso fresco-type cheese and raw milk cheese to 165F or until steaming hot. FDA has an ongoing strategy to prevent Listeria outbreaks linked to queso fresco-type cheeses.
CDC reviewed outbreak data for the raw milk cheddar cheese outbreak and other recent outbreaks linked to raw milk cheeses, which helped identify a need for consumer data to guide messaging efforts.
CDC also helped develop a consumer survey examining demographic characteristics of people who buy raw milk cheese and assessing consumer knowledge, including whether people understand if they are buying raw or pasteurized milk cheese, whether they read cheese labels, and their perceptions around the safety of raw and pasteurized milk cheeses. These survey data can be used to develop educational materials to help consumers make informed purchasing decisions.
Possible multistate outbreaks
This analysis includes investigations of 203 possible multistate enteric (intestinal) outbreaks caused by Salmonella, Shiga Toxin-Producing Escherichia coli (STEC), Listeria monocytogenes, or Campylobacter during 2024. Some possible outbreaks were excluded from this report because they were determined to be single state outbreaks or linked to international travel. After evaluation, 62 (31%) of these were determined to be multistate outbreaks, and investigators solved 45 (73%).
Multistate outbreaks
Figure 1: Number of multistate outbreaks investigated, by year and pathogen, 2016-2024*
*Investigation of possible multistate campylobacteriosis outbreaks by CDC's Outbreak Response and Prevention Branch began in 2022.
Consistent with findings of previous summaries, Salmonella caused the highest number of multistate outbreaks (38) and illnesses (2,023), making up 61% of the multistate outbreaks investigated and most (78%) of the illnesses.
In 2024, the number of multistate outbreaks investigated by CDC decreased for the first time since 2020, when the COVID-19 pandemic impacted investigation capacity. The pathogen with the most significant decrease was Salmonella, which had a 30% decrease in investigated multistate outbreaks between 2023 (54 outbreaks) and 2024 (38 outbreaks). The number of investigated Listeria outbreaks was the same between 2023 and 2024.
The 62 investigated multistate outbreaks resulted in 2,605 illnesses, 861 hospitalizations, and 36 deaths. These numbers substantially underrepresent the true number of illnesses caused by these outbreaks because many people do not seek medical care or do not get tested to see what could be causing their illness. Without testing, they cannot be identified as being part of a multistate outbreak.
Solved multistate outbreaks
Figure 2: Solved multistate foodborne and animal contact outbreaks, 2016-2024
Among the 62 investigated multistate outbreaks, 45 (73%) were solved, meaning a confirmed or suspected source of the outbreak was identified, including 28 (62%) outbreaks with confirmed sources and 17 (38%) with suspected sources.
Among the 45 solved outbreaks, 29 (64%) were linked to contaminated foods, and 16 (36%) were linked to animal contact. The percent of solved multistate outbreaks was higher in 2024 compared to 2023 (60%).
Solved multistate outbreaks caused at least 2,196 illnesses. Solved multistate outbreaks linked to contaminated food caused 1,533 illnesses, 519 hospitalizations, and 19 deaths, while multistate outbreaks linked to animal contact caused 663 illnesses, 191 hospitalizations, and 2 deaths.
Figure 3: Illnesses in solved multistate foodborne and animal contact outbreaks, 2016-2024
Outbreaks linked to food
Data summary
Age groups most at risk for severe disease
Of the 45 total solved multistate outbreaks, 29 were linked to contaminated foods. For these solved outbreaks:
- 38% had a suspected source identified
- 62% had a confirmed source identified
- 1,533 illnesses, 519 hospitalizations, and 19 deaths were reported
- 61% of ill people were female
- Ill people ranged in age from less than 1 to 99 years, with a median age of 43 years
- 5% of illnesses were in children under 5 and 26% were in adults 65 and older, which are age groups at higher risk for severe illness
- When compared with Salmonella and STEC infections, a higher proportion of Listeria infections were in adults 65 and over (64% compared to 24% and 19%, respectively).
Figure 4: Solved multistate foodborne outbreaks, by year and pathogen, 2016–2024
Demographic data
Of the 29 total solved foodborne outbreaks, race and ethnicity data were reported for 1187 (77%) ill people. Of those,
- 861 (73%) were White race (non-Hispanic)
- 169 (14%) were Hispanic or Latino ethnicity
- 99 (8%) were Black or African American race (non-Hispanic)
- 40 (3%) were Asian race (non-Hispanic)
- 9 (1%) were American Indian or Alaska Native race (non-Hispanic)
- 0 were Native Hawaiian or Pacific Islander race (non-Hispanic)
- 9 (1%) people reported multiple races (non-Hispanic)
Figure 5: Percent of ill people in solved foodborne outbreaks by reported race and ethnicity, 2024 (n = 1,187)
Foodborne outbreaks by pathogen
Salmonella caused most of the solved multistate foodborne outbreaks with 13 outbreaks (45%), followed by STEC with 8 outbreaks (28%), Listeria with 7 outbreaks (24%), and Campylobacter with 1 outbreak (3%).
Figure 6: Solved multistate foodborne outbreaks during 2024, by pathogen
Foodborne illnesses by pathogen
Foodborne Salmonella outbreaks caused more illnesses per outbreak (median: 36 illnesses, range: 9–551) compared to outbreaks caused by STEC (median: 20.5 illnesses, range: 8–104), Campylobacter (one outbreak with five illnesses), and Listeria (median: 4 illnesses, range: 2–65).
Figure 7: Illnesses in solved multistate foodborne outbreaks, 2024
As in previous years, illnesses associated with solved multistate foodborne Listeria outbreaks were more severe than outbreaks caused by other pathogens.
Overall:
- 93% of people in Listeria outbreaks were hospitalized and 13% died
- 31% of people in multistate Salmonella outbreaks were hospitalized and <1% of people died
- 41% of people in STEC outbreaks were hospitalized and 1% died
- 67% of people in the one investigated Campylobacter outbreak were hospitalized and 0% died
Pregnant women are considered a high-risk group for listeriosis, which can lead to fetal loss. In total, 11 pregnant women were part of listeriosis outbreaks in 2024. There were 4 (36%) fetal losses reported from those pregnancies. Hemolytic Uremic Syndrome (HUS) is a possible complication of STEC infection. Of the 245 ill people in 2024 STEC outbreaks with available information, 16 (7%) reported HUS.
Figure 8: Hospitalizations in solved foodborne outbreaks
Figure 9: Percentage of ill people who were hospitalized in solved foodborne outbreaks, by pathogen, 2024
Food categories
Seeded vegetables caused the most illnesses
CDC's Outbreak Response and Prevention Branch (ORPB) assigned food categories for specific foods linked to outbreaks based on the Interagency Food Safety Analytics Collaboration (IFSAC) categorization scheme.
- Vegetable row crops, dairy, and chicken were identified as the source of the most solved foodborne outbreaks (4 each) during 2024.
- Leafy greens were the product identified in all 4 outbreaks due to vegetable row crops, accounting for 127 illnesses, 53 hospitalizations, and 1 death.
- Outbreaks due to chicken accounted for 48 illnesses, 7 hospitalizations, and no deaths. Chicken liver was specifically identified in 1 of the chicken outbreaks.
- Cheese was the product identified in all 4 outbreaks due to dairy, including queso fresco style cheeses (two outbreaks), Ecuadorian cheese, and raw milk cheese. These outbreaks accounted for 43 illnesses, 33 hospitalizations, and 2 deaths.
- Seeded vegetables were identified as the source for 3 outbreaks (2 associated with cucumbers and 1 with jalapenos) and accounted for the most illnesses out of any food category, with 754 illnesses, 202 hospitalizations, and 1 death. This is almost 5 times more illnesses than the next highest food category, which was root/underground vegetables, which accounted for 152 illnesses, 53 hospitalizations, and 2 deaths.
- The 2 outbreaks due to "other meat, not poultry" were both Listeria outbreaks and accounted for 68% (13/19) of all deaths from solved foodborne outbreaks.
- The outbreak that was categorized in the "Other" category included fresh pico de gallo, but the contaminated ingredient in the pico de gallo was not identified.
Figure 10: Solved multistate foodborne outbreaks by food category, 2024
Figure 11: Number of illnesses associated with solved multistate foodborne outbreaks, by food category, 2024
Outbreaks linked to animal contact
Data summary
Animal contact linked to more illness in young children
Of the 62 multistate outbreaks investigated in 2024, 16 were linked to contact with animals or animals' food. Of the 16 animal contact outbreaks:
- 6 (38%) had a suspect vehicle and 10 (63%) had a confirmed vehicle
- 663 illnesses, 191 hospitalizations, and 2 deaths were reported
- During 2024, Salmonella caused all 16 zoonotic outbreaks
- Ill people ranged in age from less than 1 to 93 years, with a median age of 32 years
- 26% of illnesses occurred in children younger than 5, and 18% occurred in adults aged 65 and older
- Over half (54%) of ill people were female
Demographic data
Of the 506 (76%) ill people with available information:
- 363 (72%) were White race (non-Hispanic)
- 91 (18%) were Hispanic or Latino ethnicity
- 34 (7%) were Black or African American race (non-Hispanic)
- 10 (2%) were Asian race (non-Hispanic)
- 3 (1%) were American Indian or Alaska Native race (non-Hispanic)
- 1 (<1%) was Native Hawaiian or Pacific Islander race (non-Hispanic)
- 4 (1%) people reported multiple races (non-Hispanic)
Figure 12: Percent of ill people in solved zoonotic outbreaks by reported race and ethnicity, 2024 (n=506)
Illness data
Among all multistate animal contact outbreaks, 35% of ill people were hospitalized and 2 (<1%) died.
Animal sources
Contact with backyard poultry was linked to 11 solved multistate outbreaks, 532 illnesses, 145 hospitalizations, and 2 deaths. Similar to previous years, animal contact outbreaks linked to contact with backyard poultry outnumbered those linked to all other animal sources combined. However, this represents a 53% reduction in illnesses compared to 2023 and the first time since 2018 that less than 1,000 illnesses were linked to backyard poultry-associated outbreaks. Backyard poultry, such as chickens, ducks, geese, and turkeys can carry Salmonella even if they appear clean and show no signs of illness.
Small turtles (<4 inches in shell length) caused the second highest number of multistate outbreaks linked to animal contact, despite the federal ban on their sale as pets. The 3 multistate outbreaks linked to small turtles in 2024 caused 77 illnesses, 29 hospitalizations, and no deaths. Children under 5 accounted for 33% of the illnesses. Although any turtle can carry Salmonella germs that can spread and make you sick, turtles with shells less than 4 inches long are a known source of illness.
The other 2 solved multistate outbreaks linked to animal contact were caused by small mammals (feeder rodents) and squamates (scaled reptiles including lizards).
Figure 13: Total Number of Illnesses from Multistate Animal Contact Outbreaks linked to Backyard Poultry, 2016-2024
Figure 14: Number of outbreaks associated with solved multistate animal contact outbreaks, by animal contact category, 2024
Figure 15: Number of illnesses associated with solved multistate animal contact outbreaks, by animal contact category, 2024
What's being done
When investigators find the food or animal source of a multistate outbreak, agencies can take actions, such as issuing outbreak notices or requesting that companies recall adulterated products. Warning the public quickly about contaminated foods or animal contact outbreaks can prevent illnesses and save lives. Not every outbreak with a confirmed source results in product actions or outbreak notices. Outbreaks may end by the time the source is confirmed, or investigators may determine that the contaminated food is no longer available for sale.
CDC outbreak notices
Online impact
In 2024, CDC issued outbreak notices for 15 investigations. The 15 investigations included
- 12 linked to contaminated foods
- 8 resulted in food recalls
- 2 resulted in the food item not being sold temporarily
- 3 linked to animal contact or pet food
CDC uses social media and news media to further disseminate outbreak advice to the public. In 2024, outbreak posts on CDC's Instagram, X (previously Twitter), and Facebook received more than 33 million impressions in total. A Facebook post about a Listeria outbreak with a source of queso fresco and cotija cheese received over 300,000 total engagements.
Learn how CDC communicates about outbreaks
Methods
The data sources and methods used for the analyses in this report have been previously described in detail in the previous "Summary of Possible Multistate Enteric (Intestinal) Disease Outbreaks from 2017–2020" and in the MMWR report of 2016 data. Briefly, CDC maintains an internal tracking database in the System for Enteric Disease Response, Investigation, and Coordination (SEDRIC) of investigations coordinated by CDC of possible multistate outbreaks caused by Salmonella, Shiga Toxin–Producing Escherichia coli (referred to as STEC for simplicity throughout this report), Listeria monocytogenes (referred to as Listeria throughout this report), and Campylobacter. Investigation of possible multistate outbreaks of Campylobacter started being included in this summary in 2022. These analyses were based on data available in SEDRIC on June 3, 2025, and may differ from previously published reports.
An investigation of a possible multistate outbreak was included in this report if it began on or after January 1, 2024, and ended on or before March 31, 2025; or if it began before 2024 but ended between April 1, 2024, and March 31, 2025. For outbreaks linked to specific foods, outbreak vehicles were provisionally assigned food categories based on the fourth-level IFSAC categorization scheme.
These data may not reflect all of ORPB's outbreak investigation activities as some enteric pathogen strains are categorized as reoccurring, emerging, or persisting (REP) strains. REP strains can reoccur and periodically cause acute outbreaks. They can also emerge and increase in frequency or persist and cause illnesses over periods of months or years, despite investigation and prevention efforts.
Outbreak illnesses represent a small proportion of all enteric illness. People who are sick with an enteric illness may not seek medical care or be tested for enteric pathogens. Similarly, race and ethnicity data presented in this report represent those who had access to care, sought care, and had testing performed for enteric pathogens. Race and ethnicity data was missing for 23% of solved outbreak illnesses.
The number of multistate outbreaks reported here will differ from the number of outbreaks reported in CDC's Foodborne Disease Outbreak Surveillance System (FDOSS) and Animal Contact Outbreak Surveillance System (ACOSS), which include both single state and multistate outbreaks and a larger group of pathogens. In addition, the investigation year in this report, which is based on when CDC investigated the possible outbreak, may differ from the outbreak year in FDOSS and ACOSS, which is based on when outbreak-associated illnesses occurred. ORPB provisionally assigned IFSAC food categories to outbreaks in this report. Final IFSAC food category assignments for both single state and multistate outbreaks are made during the annual FDOSS outbreak closeout process.
Acknowledgements
This work would not be possible without the collaboration and critical work of many partners, including state, local, tribal, and territorial health and agriculture departments; the PulseNet database team, CDC; the Outbreak Response and Prevention Branch (ORPB), CDC; U.S. Food & Drug Administration's Office of Coordinated Outbreak Response, Evaluation & Emergency Preparedness and Center for Veterinary Medicine; and the U.S. Department of Agriculture's Food Safety and Inspection Service Office of Public Health Science, Applied Epidemiology Staff. We would like to also acknowledge Grace Vahey, Laura Gieraltowski, Kate Varela, Marisa Wong, Kathy Benedict, Kate Marshall, Colin Schwensohn, Zach McCormic, Misha Robyn, Alondra Báez, Lauren Gollarza, and Sarah Collier (ORPB) for their efforts during the writing of this report.